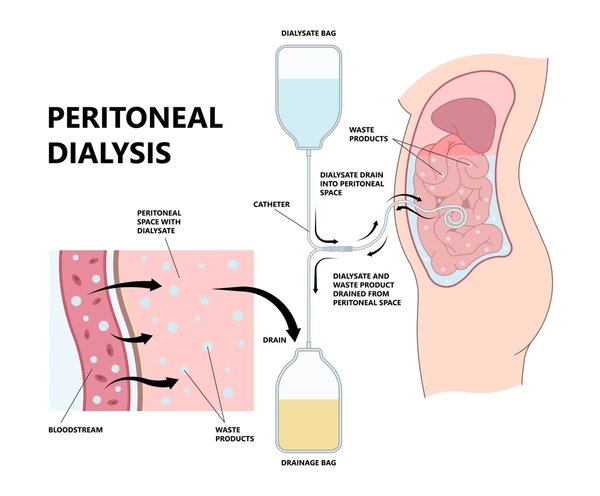
What is Peritoneal Dialysis?
Peritoneal dialysis is a treatment that uses the lining of the peritoneum inside the abdomen to filter waste, excess fluids, and toxins from the blood. Unlike hemodialysis, which relies on a machine, PD uses a sterile solution called dialysate that is introduced into the abdomen through a catheter. The solution absorbs waste and excess fluids from the blood vessels in the peritoneum, and after a few hours, it is drained away, carrying the waste with it. A nephrologist carefully guides patients through this process to ensure safe and effective treatment.
Types of Dialysis
There are two different modalities of dialysis, Haemodialysis or peritoneal dialysis. In haemodialysis, blood is filtered through a machine outside the body. For peritoneal Dialysis, a cleansing liquid is infused through a catheter into the peritoneal cavity:
Continuous Ambulatory Peritoneal Dialysis (CAPD)
This method is manual and performed by the patient or a caretaker 4-5 times daily and once at night. The patient will fill their abdomen with dialysate, let it stay for a few hours to absorb waste, and then drain it out.
Automated Peritoneal Dialysis (APD)
This is done with the help of a machine (cycler) that performs the exchanges, like putting fluid into the cavity and removing it several times overnight. The patient is free of the fluid during the day time, making it a convenient option for patients.
How Peritoneal Dialysis Works?
Dialysate Infusion
A sterile fluid (dialysate) is introduced into the abdominal cavity through a Peritoneal Dialysis Catheter
Waste Removal
The dialysate absorbs waste products and excess fluids from the blood vessels in the peritoneal lining.
Draining the Fluid
After a set period, the used dialysate, now filled with waste, is drained out of the abdomen and replaced with fresh fluid.
Benefits of Peritoneal Dialysis
Risk & Considerations
- Infection: Since PD involves a catheter in the abdomen, there is a risk of infection, particularly peritonitis. Proper hygiene and care are essential.
- Fluid Balance: It’s important to monitor fluid intake and output to avoid overload.
- Potential for Weight Gain: High glucose in dialysis solution can lead to weight gain.
- Training and Support: Patients and caregivers must be trained to perform exchanges and care properly.
Lifestyle Considerations
1
Dietary Management
Follow a kidney-friendly diet low in sodium, potassium, and processed foods.
2
Exercise
Maintain regular physical activity to improve overall kidney and heart health.
3
Mental Health
Manage stress and seek emotional support to improve treatment outcomes.
4
Regular Checkups
Routine monitoring helps detect issues early and ensures effective care.
Get More Consultations
Take the first step towards better kidney health with expert nephrology care from Dr. Kosha Patel. Manage chronic kidney failure confidently with compassionate, specialized treatment tailored just for you.
Contact Us
